Active substances for leaky gut
Why many diseases of our modern society could have their origin in our intestines
Dr. med. Heinz Lüscher
Can it be that many chronic diseases, not only the typical intestinal diseases, but also allergies, hypersensitivities, metabolic diseases and autoimmune diseases have their origin in the intestines? Are there highly interesting interrelationships which, in their scope, are almost life-shaping for our modern society and which, if better understood, could even make it possible for seemingly chronic diseases to become treatable? What sounds a bit far-fetched at first, we now may be able to shed some light on. Let us take a closer look!
Our Gut – a miracle machine
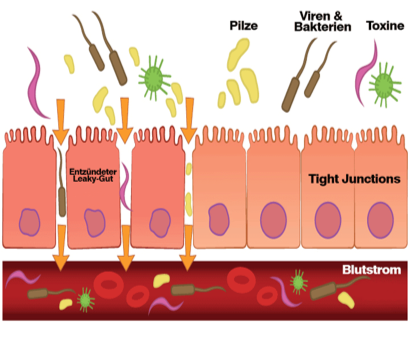
So, let us start our journey through the intestine, or more precisely the intestinal wall. The intestinal surface, with its multidimensional protuberances, provides an impressively massive surface area, comparable to a tennis court! The different intestinal cells have a multitude of functions, with the absorption of the previously digested nutrients being the most important. The healthy intestinal wall serves on the one hand as a barrier to protect the body from infections, yet on the other hand must also allow permeability, so nutrients can be absorbed by the body. If the intestinal wall is irritated or inflamed, these functions are severely impaired. The result is the so-called Leaky Gut Syndrome, where an irritated or damaged intestinal wall, allows an increased permeability for all substances, good and bad.
Immune System
The intestinal wall is, so to speak, the largest interface between the body and the outside world. Is here that the rules must be determined regarding foreign substances are allowed to pass and which need to be prevented. The immune system, of which around 70% is made up of the intestine, therefore plays an extremely important role as a controlling authority. The innate immune cells with their special receptors enable the immediate detection of intrusive toxins. So-called endotoxins, also called lipopolysaccharides (LPS), are decaying products of gram-negative bacteria that can trigger numerous pathological reactions in humans when they penetrate the intestinal wall and enter the bloodstream!
The’Leaky -Gut’
At this point we come back to the previously mentioned Leaky-Gut. This is, as the name suggests, an increased permeability of the intestinal wall to certain substances, the otherwise tight closure of the intestinal cells (tight junctions proteins) fails and food components can pass through. This can cause intolerances, but even more problematic is that LPS (lipopolysaccharides) enter the bloodstream through the intestinal wall, which can have catastrophic consequences throughout the body.
The formation of a Leaky Gut from right to left:
The securetight closure of the tight junctions proteins is damaged, allowing the passage of food components and LPS into the bloodstream
The Immune Response
The increased penetration of undigested food components and bacterial toxins causes an immune response. The cells of the innate immune system (macrophage, dendritic cells, granulocytes) as well as the thrombocytes recognise and bind the bacterial toxin LPS via the Toll-like receptor 4 (TLR4). The TLR4 is the docking site for LPS on the cell membrane. The docking of these substances to these immunocompetent cells leads to incompatibilities and inflammatory reactions.
Inflammatory response
The persistence of such an inflammatory reaction results in a shift of the immune imbalance between the innate and acquired immune system. This can lead to allergic food intolerances or inflammatory diseases. Chronic inflammations are counteracted over the course of time by counter regulation, which in turn can lead to disorders of the immune system’s competence with the corresponding clinical outcomes.
Inflammation is basically seen as a positive process, with which our body wants to lead to healing through increased blood circulation and water retention and selective overheating.
If, however, our organism is busy with many inflammations, it can result in excessive immunological reactions, including the misdirection of the attack towards one’s own tissue structures with the result of autoimmune diseases.
The function of the Thrombocytes
How exactly do the LPS get into the entire body? This is mainly due to the thrombocytes that are known for their coagulation functions and whose surface contains more than 200 receptor types.
The LPS are recognized by the platelet at TLR4 and bind to it. The thrombocyte changes its shape, becomes more fragile and then can burst if the load is too high. This happens mainly in two places in the body; 1. in the liver attributed to alkaline phosphatase and 2. in the heart by the shearing forces caused during the pumping process. The destruction of the thrombocytes releases pro-coagulative and pro-inflammatory cytokines as well as, the LPS, which now causes an immunological emergency reaction, as the tissue now must assume there is a local bacterial infection. Since the TLR4 is found in very different cell types in the entire body, the released LPS can now dock on in numerous places, at will.
The microbiome
It becomes clear that a healthy, irritation-free intestinal wall is essential for a stable immune balance, so that it can (again) fulfil its barrier function! Let’s look again at what is happening in the intestine. In here thousands of “good” bacteria of different species work together in a symbiosis. What used to be called intestinal flora is now usually referred to as microbiome. The microbiome could almost be described as an organ in its own right. It consists of about 100 billion bacteria (many times more than all human cells!) from over 1500 different bacterial species and weighs about 2 kg. These industrious helpers break down the food and make it digestible for us. They also produce amongst other things, certain vitamins, such as vitamin K and B vitamins, they also produce digestive enzymes and hormones. Depending on the intestinal segment, there are special types of bacteria that maintain the function and environment of that specific area. The whole process is under permanent surveillance and control of the immune system. An interplay takes place; a balanced intestinal flora promotes our well-being, but our state of health in turn also influences the intestinal flora.
The role of the Cytokines
The cytokines play a special role, these signal molecules form the direct influence on control, regulatory circuits, cell reactions, escalation and de-escalation mechanisms, signal transmission, initiation of emergency measures and much more.
If LPS is now recognised and absorbed by the immune cells within the framework of a leaky gut, the immune response cascade begins and the activated immune state in turn links back to the state of the microbiome, because it is also under the influence of the cytokines.
The chain reaction is called the Leaky-Gut syndrome:
LPS-Invasion➔ Immune Escalation ➔ Cell and Organ Damage and the resulting vicious circle is the net result.
The basis of this writing was the technical contribution “The cycle of inflammation – Are our diseases of civilization possibly in an unrecognised context?” by Drs. Henry Krah & Marcus Stanton.
Effective treatment of a leaky gut
But how do you get out of this cycle, is that even possible?
With a special combination of high-quality vital substances, one could support the body significantly in its recovery. However, in the case of leaky gut syndrome, these substances can unfortunately only be absorbed to a limited extent due to the irritated intestinal wall and therefore do not lead to the desired success on their own. It must be a product that on the one hand contains a high concentration of certain vitamins and secondary plant substances (vitamin C, vitamin B12, quercetin, vitamin E, folic acid, beta-carotene, alpha-lipoic acid), but on the other hand also has a special transport system that makes absorption in the damaged intestinal villi possible at all. Thanks to a technical tour de force by a medical company in Germany, it has been possible to make exactly this possible. Thanks to a sophisticated, patented process, the ingredients enter the blood and the body’s cells despite the inflamed intestinal mucosa. This product additionally but also highly effectively supports the regeneration of the inflamed and damaged intestinal wall, thus breaking the cycle of Leaky Gut. In addition, the intestine should be supported with further measures. These include a detoxifying product such as clinoptilolite, an anti-inflammatory such as turmeric, vitamin D3 and omega-3 fatty acids, and a high-quality prebiotic.
Diagnosis Leaky-Gut
Diagnosing a leaky good is very easy with the Panda test (platelets adhesion by number of different anticoagulants) developed and validated by Prof. Dr. med. Götz Nowak, University of Jena, Germany
For this one needs the following 2 blood analyses
- platelet count in the heparin tube
- platelet count in EDTA tube
Conclusion:
In conclusion – If there is a deviation of more than 10% between the two analyses (the value of the heparin tube is lower), this is evidence that polysaccharides are entering the blood through an inflamed intestinal wall. Subsequently, a diagnosis of Leaky-Gut is given. The greater the difference between the two test counts, the stronger the indication. If the difference is more than 25%, we call this a severe Leaky-Gut syndrome.
Other nutrients
Who should be checked for Leaky Gut?
When should Leaky-Gut be considered as a possible cause of illness? Who should be recommended to undergo an assessment?
As already mentioned, a leaky good can lead to a long list of chronic diseases such as allergies, intolerances, metabolic diseases and autoimmune diseases. In these cases, a leaky good should always be considered as a possible cause. Chronic digestive problems and gastrointestinal complaints, fatigue, sleep disorders and loss of energy, depressive moods and susceptibility to infections can also point to this diagnosis. Usually there is a combination of different diseases, symptoms and a long history of suffering and illness.
As a leaky gut can develop as a result of our modern lifestyle with a lot of stress (distress), industrially changed foods and numerous environmental toxins, a healthy, varied and high-quality diet and a balanced lifestyle form one part of a preventative treatment (prophylaxis) and is also the indications for the treatment of a leaky gut.
